FGF21 – a liver hormone linking sugar cravings and cardiovascular disease.
On Christmas Eve the media carried reports that scientists had identified a hormone, produced by the liver, that switches off sugar cravings, and which might be the answer to sugar addiction.
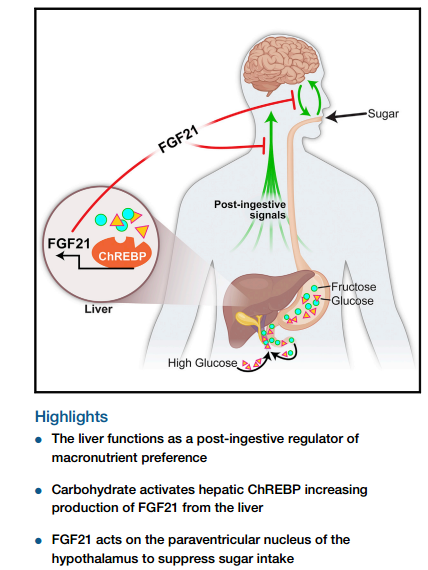
“Research on mice and monkeys has shown that the hormone, FGF21, signals the brain to avoid seeking sweet foods.
Harnessing the effect, possibly by copying the hormone’s action with a drug, could help patients who are obese or suffering from Type 2 diabetes, scientists believe.”
We all know that a LCHF diet suppresses the appetite for sugar – one of my dietary epiphanies involved standing in a supermarket, among shelves of garishly packaged chocolates and sweets, and realising that though being exposed to that stuff had always obliged me to buy some piece of it to take away and eat before, now I hadn’t a single impulse worth fighting to buy or eat any of it ever again.
So it was an obvious question (one I may not have asked had I read the full paper first, because in the actual experiment FGF21 is clearly being produced in response to eating carbohydrates) whether a ketogenic diet raises FGF21.
It does – FGF21 is part of the regulatory response to fasting or a ketogenic diet (in mice).
So, eat keto, and your liver produces FGF21, which stops you wanting sweet food. Simple.
But, like that book by Ben Goldacre, I think you’ll find it’s a bit more complicated than that.
Luckily though, the complexity of FGF21 seems to fit a pattern we’ve seen before with other hormones.
While I was looking for the link to ketosis, I noticed in my search results a paper linking elevated FGF21 to cardiovascular disease. How can something that stops you from eating sugar be linked to CVD? That was before I knew that FGF21 was produced in response to eating carbohydrates. By the time I read the CVD paper, I knew what I was looking for. Here it is; The metabolic syndrome has also been associated with increased serum FGF21 levels, whereas an increase in FGF21 serum levels has been suggested as a new biomarker for nonalcoholic fatty liver disease or steatohepatitis (17, 54, 60, 62, 116, 118). A study on obese children confirmed that increased serum FGF21 is correlated to BMI and free fatty acids (90). When serum FGF21 levels were tested after an oral load of fructose, it was interestingly shown that FGF21 values
acutely spike, presenting a similar curve as serum glucose and insulin after a glucose load. This finding shows that FGF21 presents a typical hormonal response possibly mediated by carbohydrate-responsive element-binding protein that is activated by fructose (18).
…it was shown that FGF21 levels are predictive of combined cardiovascular morbidity and mortality (Fig. 3) (59). Increased baseline serum levels of this molecule were found to be associated with a higher risk for cardiovascular events in patients with type 2 diabetes in the Fenofibrate Intervention and Event Lowering in Diabetes (FIELD) study, and interestingly this association tended to be stronger in the patient group that presented higher total cholesterol levels (84). The authors speculate that the increased basal levels of FGF21 in this group of patients may be an indication of the potential role of FGF21 as a biomarker for the
early detection of cardiometabolic risk and furthermore that it may reflect a compensatory response or the need of supraphysiological doses of FGF21 as a result of FGF21 resistance, a hypothesis proven in obese mouse models (21).
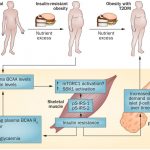
FGF21 resistance and hyperFGF21aemia. It’s a familiar pattern. If FGF21 is produced in response to carbohydrate – maybe when hepatocytes reach glycogen saturation or ATP depletion or some other threshold – but your lifestyle or culture involves eating past the signal, maybe because of some dopamine effect of sugar you’re sensitive to, or because you bought the 1.5 litre bottle of Coke because it was cheaper than the 300ml and it shouldn’t go to waste, or because your mum or dietitian is telling you to finish your cake or keep eating the low fat food regularly, then maybe your liver eventually, because you stopped listening to it, makes so much FGF21 that the cells that should notice it become insensitive to it, so you eat more sweet carbs, make more FGF21, and get the same vicious cycle that we see with insulin.
(Or maybe there’s some other cause for FGF21 resistance, a virus or environmental toxin or food colouring or genetic bad luck. It doesn’t really matter unless you finish the cake.)
So what happens when a modern human goes on a keto diet or fasts? FGF21 may not rise at all – instead, sensitivity can be restored by its dropping, much like insulin.
Raymund Edwards astutely tweeted this study, which shows what happens to FGF21 when humans fast for 10 days. It’s not the same as it was with the mice. In the mice on the ketogenic diet, it sometimes looked as if FGF21 played a role in ketogenesis – in the fasting humans, ketones rose first and FGF21 followed days later. This actually makes more sense, because ketones suppress appetite independently of FGF21, and are produced through basic biochemical economics – this shouldn’t require some fancy new hormone, just let glucagon dominate over insulin and the Krebs cycle will do the rest.
In some of the humans, FGF21 was elevated at baseline and dropped fairly quickly, as can be seen in the spaghetti plot:

Whereas ketones rose more rapidly:
Anyway, this line of investigation, which I have only skimmed superficially here, gives us two possibilities; we have pathways which we can use to explain the loss of a sweet tooth when carbs are restricted (either FGF21 elevation, or the restoration of FGF21 sensitivity), and, we have an additional connection between sugar and cardiovascular disease.
What does it mean that FGF21 rises so much when fasting (and probably similarly on a keto diet), if elevated FGF21 is associated with CVD and other metabolic diseases?
If you read the CVD paper, FGF21 has a number of beneficial and antiatherogenic properties. It doesn’t seem like bad stuff to have elevated, unless it got that way from a high intake of fructose.
http://hopefulgeranium.blogspot.ca/2015/12/fgf21-liver-hormone-linking-sugar.html